A major factor that leads to bone degradation and how Ayurveda can tame it

Some years ago, Gwyneth Paltrow got a lot of grief and ridicule for calling her separation from her then-husband Chris Martin “conscious uncoupling.” I personally think that it’s a very descriptive term, and it seems like conscious uncoupling would be more mature than the unconscious one. But I am more fascinated by the term uncoupling, which, to me, conveys the separation of two parts that are meant to be together, with all the grief and heartache involved. Uncoupling can also happen within our bones, and it can also cause all sorts of problems to our bones and bodies in general.
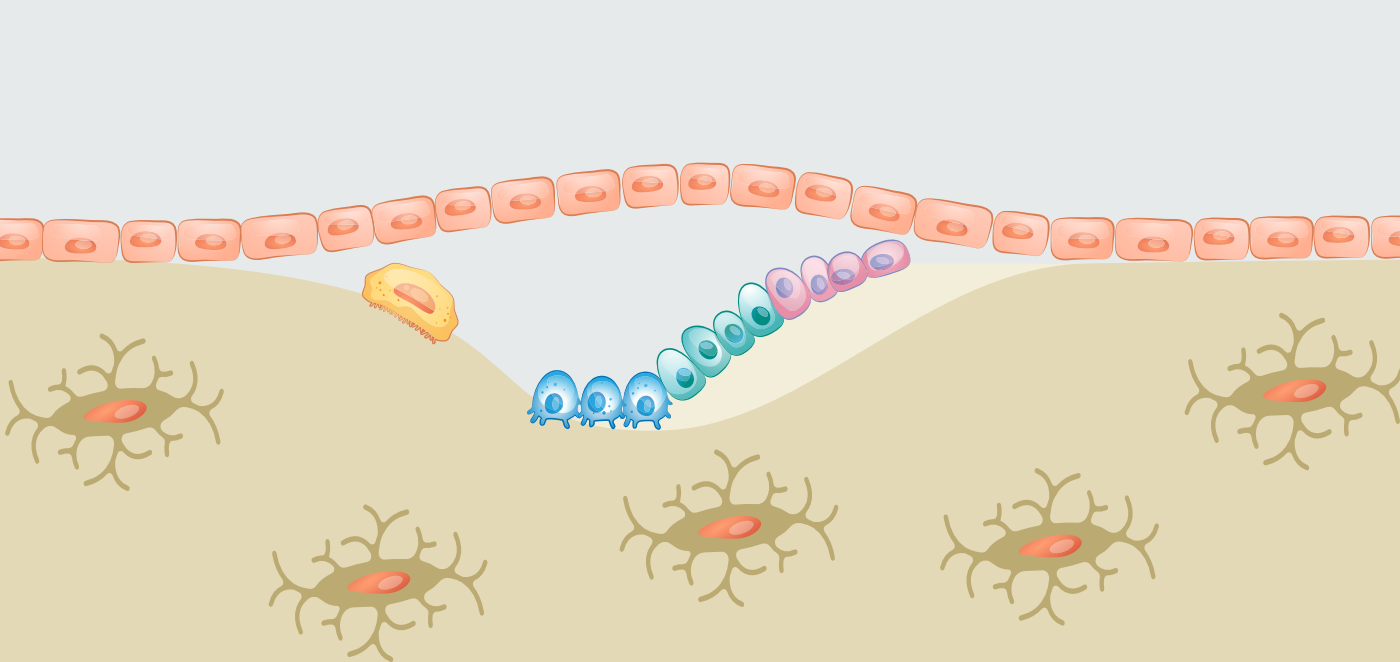
Our bones are fascinating entities that constantly renew and remodel themselves. The process of bone remodeling is mainly conducted by three types of cells: osteoclasts (bone breakdown), osteoblasts (bone formation), and osteocytes (supervision), and is facilitated by a variety of hormones. Here is a quick review of what it looks like (read a more detailed description here >).
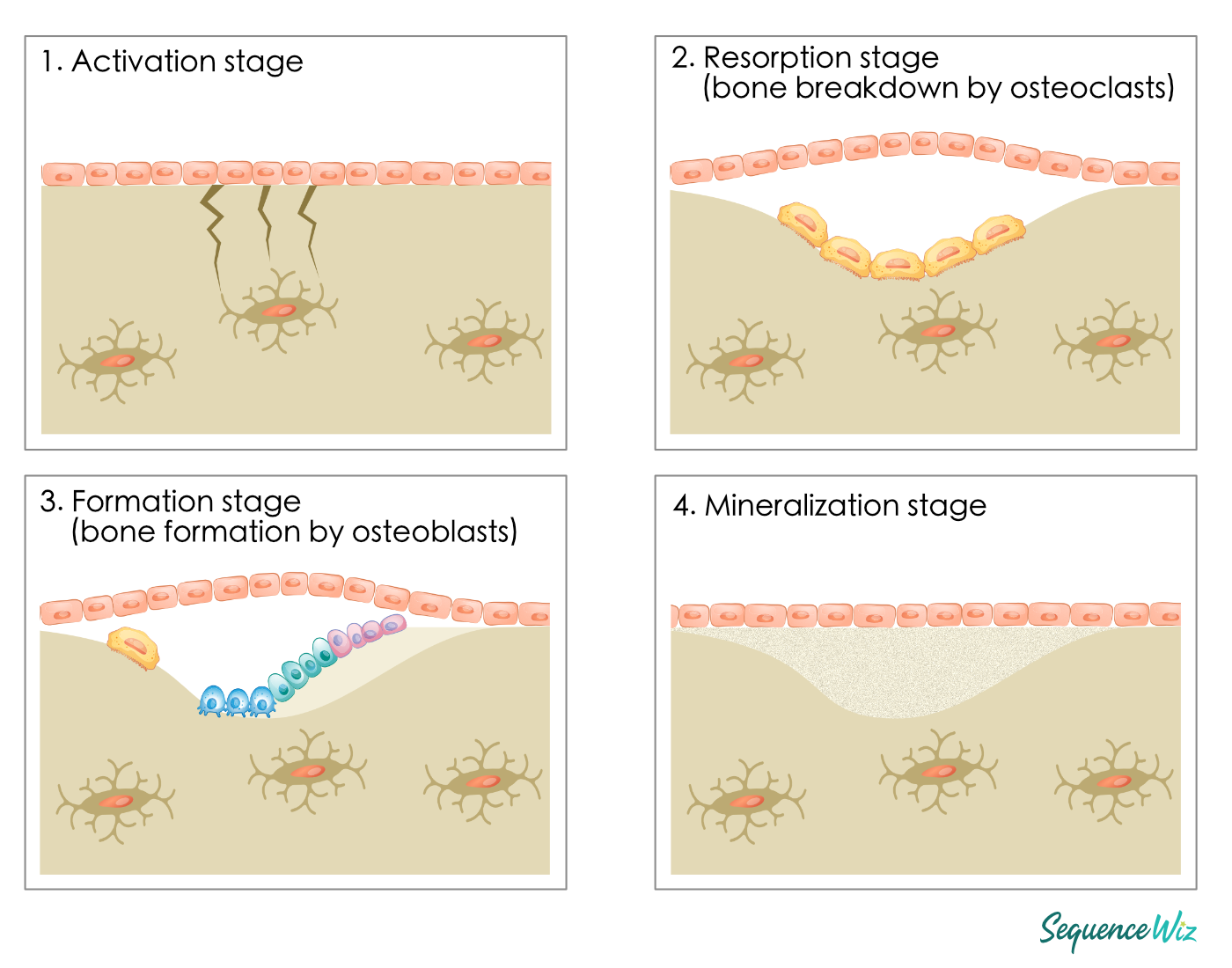
The actions of the osteoclasts (bone breakdown) and osteoblasts (bone formation) are closely linked and referred to as a coupled process. It is essential to balance the amount of bone being removed and that which is being formed. If this process becomes uncoupled, there will be too much bone breakdown and not enough formation, leading to bone mass loss. Many factors come into play in this delicate process. There is one additional factor that is frequently overlooked, and that factor is inflammation.
Inflammatory diseases can arise all over the body, including in the musculoskeletal system (for example, rheumatoid arthritis), the intestines (for example, inflammatory bowel disease), the oral cavity (for example, periodontitis), and the lungs (for example, cystic fibrosis). To deal with inflammation, the body releases various cytokines, small proteins that control the growth and activity of other immune cells and blood cells. When released, cytokines signal the immune system to do its job. Unfortunately, if the inflammation continues for an extended time, high levels of cytokines lead to hyperactivation of osteoclasts, the cells that break down bone. This means that the bone will be broken down much faster than being rebuilt. This can lead to excessive bone degradation. Dr. R. Keith McCormick, in his book The Whole-Body Approach to Osteoporosis: How to Improve Bone Strength & Reduce Your Fracture Risk, writes: “Overly aggressive osteoclasts that destroy bone quality can be compared to a horde of carpenter ants that bore a maze of destructive tunnels through a tree trunk. Just as ants tend to burrow through the trunks of sick, elderly, weakened trees, osteoclasts become aggressive in physiologically weakened bodies.” (1) Luckily, nowadays, there are tests that can help you determine how much bone osteoclasts are destroying by testing the tiny pieces of collagen released from bones into the circulation and then excreted with urine. Your doctor can order a resorption marker test to assess the rate of bone breakdown and then monitor the effectiveness of the prescribed treatment. If you have been diagnosed with an inflammatory disease, you would need to closely monitor your bone density and take steps to keep your bones healthy and strong.
Those of us who haven’t been diagnosed with inflammatory diseases are not off the hook either. Quite often, there is low-degree inflammation happening in our bodies that doesn’t rise to the level of disease but affects our bone health all the same. Dr. R. Keith McCormick writes: “Conditions such as long-term infection, exposure to toxins, food allergies, vitamin D deficiency, abnormal overgrowth of bacteria within the gut, or even constant emotional stress can create undue pressure on the immune system. […] This distress leads to chronic low-level inflammation, a major component of many chronic diseases, including osteoporosis. […] Chronic inflammation can cause osteoclasts to become aggressive scavengers of mineralized bone. Instead of digging shallow resorption pits that the osteoblasts can easily fill with new bone, inflammation-driven osteoclasts establish a huge number of basic multicellular units [bone remodeling sites] and excavate what looks like deep miniature crevasses. Such intensive remodeling multiplies the risk of fracture.”(1) Symptoms of chronic low-level inflammation can show up anywhere in the body and may include redness, skin dryness and sensitivity, irritability, anger, fatigue, joint pain and stiffness, loss of appetite, digestive issues (constipation or diarrhea), headaches, muscle stiffness, and muscle wasting.
Looking at the list of symptoms, one might say, “Jeez, what isn’t included here?” But if we switch gears and look at those symptoms through the Ayurvedic lens, we might see a common thread (or two) running through. Half of those symptoms describe Vata (air) disturbances (skin dryness, fatigue, joint stiffness, lack of appetite, constipation, headaches, muscle wasting), and the other half reflects Pitta (fire) disturbances (redness, skin sensitivity, irritability, anger, joint pain, diarrhea, muscle stiffness). The Vata part of the equation makes perfect sense: Vata-dominant folks are constitutionally much more likely to experience loss of bone density and have a higher risk of fractures because of Vata’s inherent qualities of dryness, lightness, and subtleness. These qualities only intensify if Vata is imbalanced or when we enter the Vata stage of life (after the age of 50). But it appears that increased Pitta quality of heat (which is represented by inflammation) speeds up this process.
Let’s think of it in terms of elements. Logs of wood are made of fiber and minerals, similar to how bones are made of collagen and minerals. What would happen if you left a log in a dry, sunny place (air + fire qualities) for a while and then put it into a raging fire (air + fire qualities)? The log would burn out and become brittle. Even when the fire is timid and slow-burning, it will have the same effect on the log if it lasts long enough. Similarly, when our bones are subjected to prolonged Vata and Pitta imbalances, they dry out and become brittle and fragile. In practical terms, this means that folks who have high Vata and Pitta in their constitution are more likely to develop these sorts of problems. The risk increases if we let our inner fire rage uncontrollably. If we frame our thinking that way, the solution to the problem becomes more obvious. We would need to use all the tools at our disposal (diet, environment, lifestyle, exercise, breathing techniques, and mental techniques) to pacify both Vata and Pitta.
Although Ayurveda offers very detailed dietary suggestions to balance your constitutional type, you don’t have to follow an Ayurveda-based diet to decrease chronic inflammation. There are plenty of informative sources out there that can help you make better choices about foods that naturally fight inflammation, like this helpful and beautiful video (the entire YouTube channel Pick Up Limes is delightful and full of delicious recipes). Remember, chronic inflammation can adversely affect various levels of our systems, not just our bones.
References
- The Whole-Body Approach to Osteoporosis: How to Improve Bone Strength and Reduce Your Fracture Risk by K. McCormick (affiliate link)
- Fundamentals of Anatomy & Physiology by F. Mattini, J. Nath, and E. Bartholomew (affiliate link)
- Yoga for Osteoporosis: The Complete Guide by L. Fishman and E. Saltonstall (affiliate link)
Get yoga practices for skeletal system and many other yoga videos for digestive, respiratory, cardiovascular, nervous, and immune systems in the Zoom In Within yoga series.






Olga, what a beautifully written piece. Fabulous explanation of how the body works, and as always, clear and inspiring.
Great article and love the Pick Up Limes video. Thanks for sharing this resource.