SOAP Notes: A Structured Approach to Yoga Therapy Documentation
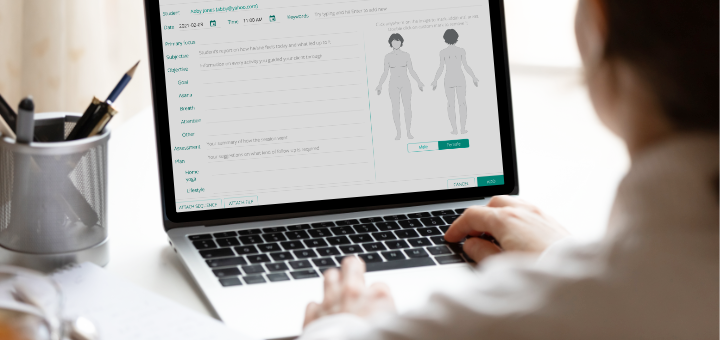
When we work with yoga students one-on-one, it is essential to keep detailed notes of our work. Those notes help us determine students’ challenges and strengths; develop an appropriate plan for our work together; record yoga practices and lifestyle recommendations to guide them; and keep track of the students’ progress. Most health care professionals write regular notes as part of their practice, but it can feel foreign and challenging for many yoga teachers and yoga therapists. That is why I asked my friend and fellow yoga teacher Erin Bookout to share her experience with writing progress notes to make it a bit more accessible and interesting. Erin is also a speech pathologist who works at the VA hospital in Portland, OR, and writes dozens of patient notes every week. Here is her take on writing progress notes. (OK)
by Erin Bookout

A common challenge in the provision of yoga therapy is documentation. How do we make our notes concise without sacrificing content? How do we make our notes clear enough that another teacher knows what we did in a session and is able to pick up where we left off? And as we, as a profession, move towards insurance reimbursement, how does our documentation satisfy reimbursement requirements and established norms?
Fortunately, there is a vetted, systematic documentation template that meets all of these needs – the SOAP note. This is a documentation template used across American medical professions that, when used correctly, facilitates efficient documentation. Some of you may have spent time in a training covering SOAP notes, and left feeling more confused about documentation than when you began. The goal of this article is to demystify the SOAP template and provide enough examples of its use in yoga therapy that you feel more comfortable using it. I am primarily addressing its use for treatment sessions rather than evaluations, as the latter should include significantly more information. You may find that, like any new clinical skill, initial use of the SOAP template takes time, but with practice and use, it can increase clinical efficiency.
SOAP OVERVIEW
I often think of my notes telling a story of sorts – the exposition (setting and characters), the plot (what happened), the moral or summary of the story, and the cliffhanger to keep the reader wanting more. This corresponds generally to the structure of the SOAP note. In this section, I’m going to provide you with a general overview of each part of the SOAP note. In the following sections, I will apply these specifically to yoga therapy.
“S” stands for “Subjective” – this is where all of the background information about the setting and characters comes in. It includes information like the history, what has happened in the interim since seeing the client last, what the client reports. It’s the exposition of your story.
“O” stands for “Objective” – this is where the data about what happens in the session goes, your treatment and the client’s response. This is the plot of your story.
“A” stands for “Assessment” – this is where you make a statement of how the session went, putting your data (“O”) in the context of the background (“S”). This is the moral or summary of your story.
“P” stands for “Plan” – this is where you state your recommendations based on the three sections above. It often includes a description of the home program that you have assigned the client. It can represent either a cliffhanger (“Next time, on yoga therapy with Erin…”) or a THE END in the case of discharge.
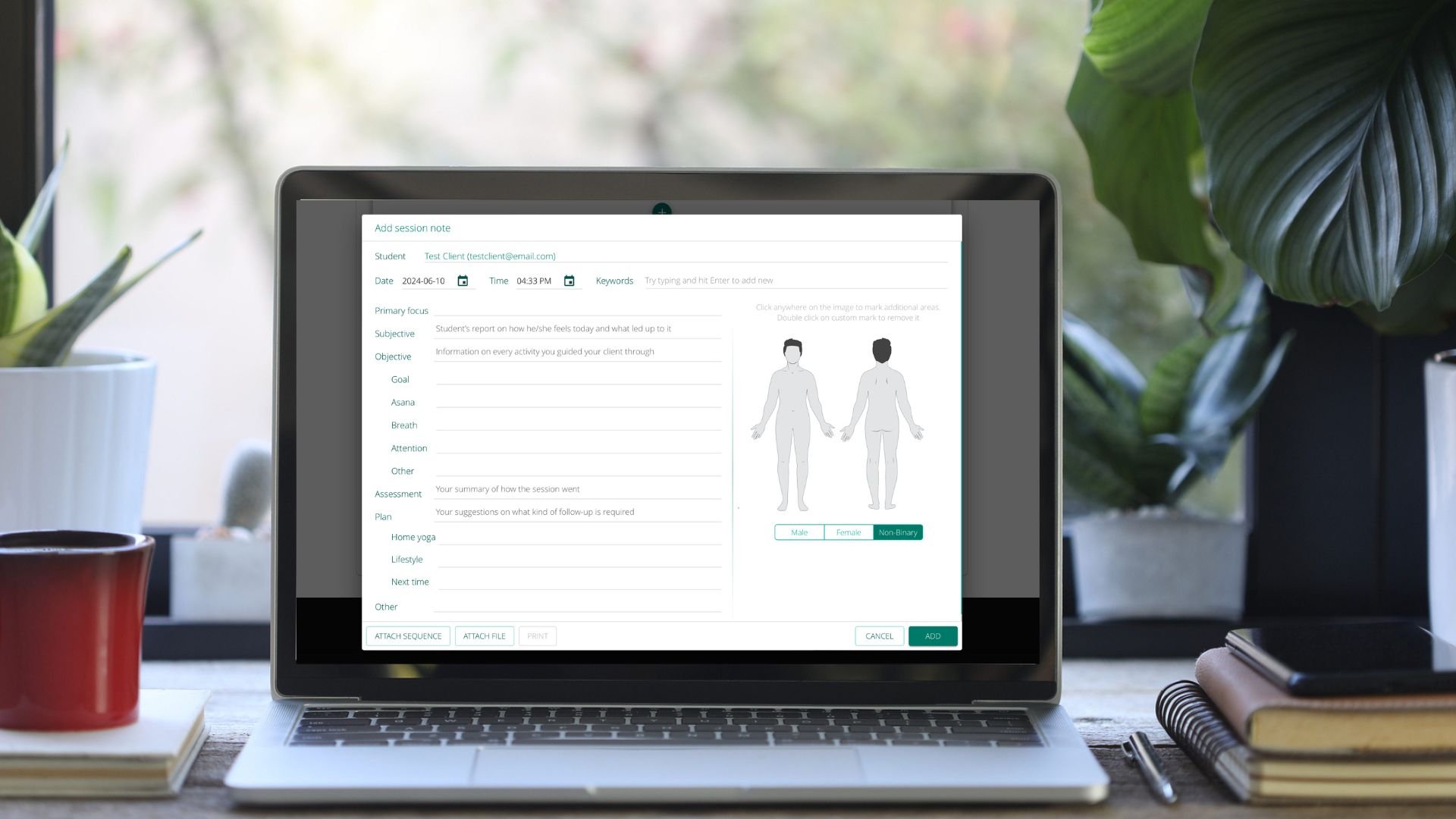
S: SUBJECTIVE
Subjective information in yoga therapy includes the reason you are seeing the client, the environment of the session, how long your session is, and what the client reports has happened since your last session.
S:
DJ was seen for a 60-minute yoga therapy session (the 2nd of 6 planned weekly session) at Portland Yoga Studio. He reported that he completed exercises every morning since our previous session one week ago. He reported confusion about arm position in the three Warrior I variations. He reported that his lower back pain decreased for several hours following completion of the sequence each time he completed it.
This is the part of your note to include information that significantly impacted the rest of your session, such as recent stressful events.
S:
MB participated in a one-hour yoga 1:1 session (#4 of 8). She denied completing any of her home program because her dog has been ill, which resulted in having to have him euthanized late last night. She reported she has not slept in three days. As a result, our session was significantly modified (see below).
Again, the Subjective section is where you set the stage for what you did in your session with the client.
O: OBJECTIVE
Objective information includes the activities you guide your client through and the response to these activities. Many find it useful to report this in terms of the goals that have been set for the client at the outset of therapy.
O:
EDUCATION
LONG-TERM GOAL 1: Client will participate in ongoing education re: breath awareness, pairing breath with movement, general anatomy and physiology of the spine, rationale for tools chosen, goal-setting and modification.
RESULTS: Client demonstrated good comprehension of all information reviewed.
COORDINATION OF BREATH AND MOVEMENT
LONG-TERM GOAL 2: Client will pair breath with movement in assigned exercise program without cues.
RESULTS: Moderate verbal cues required, particularly in seated postures.
THORACIC SPINE
LONG-TERM GOAL 3: Client will report decreased pain with aggravating activities with completion of home program.
SHORT-TERM GOAL 3A: Client will perform thoracic mobility focused home program independently.
RESULTS: Moderate verbal cues to perform full asana series (see attached); provided shortened version for home program.
Another way of reporting your data in this section is attaching the practice you led the client through and annotating the client’s response, including decreased pain, increased mental alertness, decreased anxiety, etc. This section is usually the longest of the four.
A: ASSESSMENT
The Assessment portion of a treatment note includes a summary statement of how the session went, the client’s progress in therapy so far, and adjustments that need to be made for future sessions. There should be no new information included in the Assessment.
A:
LM reported decreased hip pain following today’s session and will benefit from ongoing completion of home program. Cues to release hip flexor tension using exhalation during held postures were particularly beneficial. She has participated in five of eight planned treatment sessions and is making good progress towards goals.
P: PLAN
The Plan should logically follow from the Assessment, is typically rather brief, and includes the home program you have assigned. For example:
P:
Recommend:
1) Continue home program (attached).
2) Continue to increase walking distance as tolerated.
3) Return for session in two weeks (due to client vacation next week).
Recommendations following discharge are included in the Plan as well:
P:
Client has met stated goals and is independently completing home program. Recommend discharge from 1:1 sessions, continued completion of home program, and consideration of weekly Gentle Yoga classes to maintain gains.
It might feel a bit challenging to write SOAP notes at first, but just like any other skill, it gets better the more you practice. Over time, each practitioner develops their own writing style and personal repertoire of professional language. And since yoga teachers do not have strict standards for SOAP notes right now, you can take time to find your own voice in those notes.
Check out this 3-minute video to see how you can use SOAP notes to deepen your understanding of your student and become a better yoga teacher/therapist.
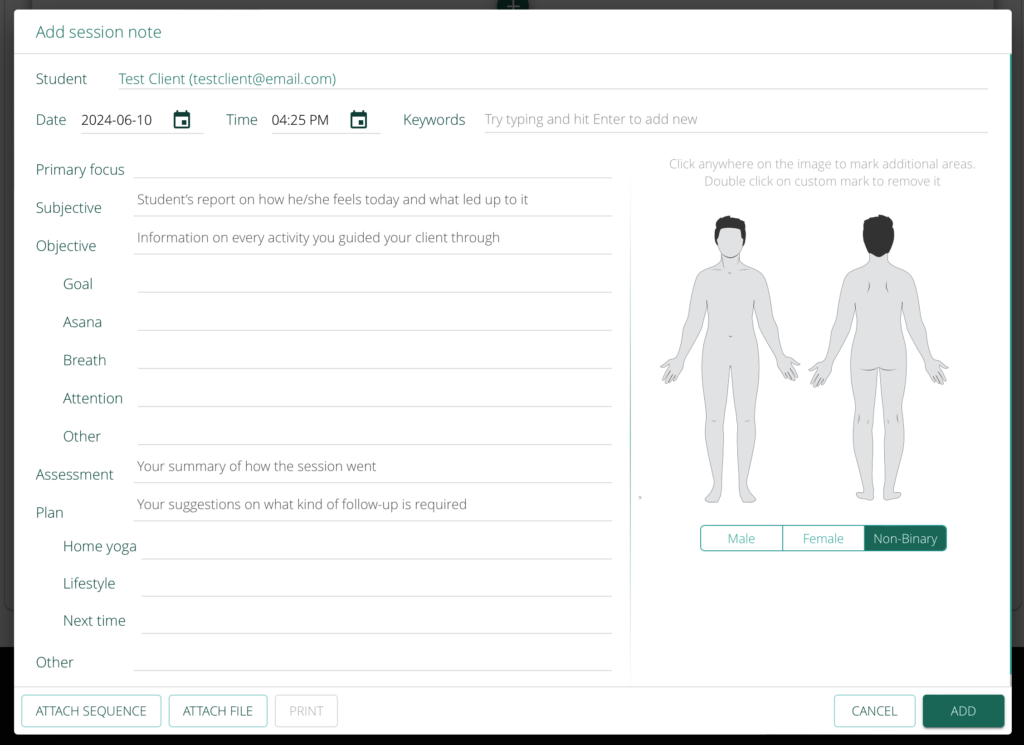
Follow a simple pattern with prompts to quickly record your SOAP notes.









This is incredibly helpful; thank you for the detailed examples.
I really can’t thank yoga therapy enough for helping me get through my cancer treatment years ago. Up until now I attend sessions over at https://revivorship.com/services/yoga-therapy/ years after I was cleared for cancer and it has really helped me relax so much!
Thank you! What program are you using in the image?
Hi Kristen! That’s our own program, Sequence Wiz Student Management System. You can read more about it here > Please let me know if you have any questions!
Thank you. Information was very helpful.
Thank you! This has been incredible helpful!
Great! Happy to hear that, Vincent!